- Hereditary Hemorrhagic Telangiectasia - May 25, 2016
- Hereditary Hemorrhagic Telangiectasia: Septal Perforation and Nose Bleeds - May 23, 2016
- Hereditary Hemorrhagic Telangiectasia: Epistaxis and Septal Perforation - May 18, 2016
- Wegener’s Granulomatosis: Autoimmune Disease and Multi-Focal Septal Perforation - May 9, 2016
- Kyle Korver: Facial Injury and Nasal Fracture - March 24, 2015
- Russell Westbrook: Facial Injury and Surgery - March 5, 2015
- Mega-perforation: Pushing the Limits of Septal Perforation Repair - November 26, 2014
- Septoplasty Complication and Septal Perforation - November 24, 2014
- Nose Picking (Rhinotillexis) and Septal Perforations: Why I should stop picking my nose…? - November 24, 2014
- Nasal Fractures, Septal Hematoma, and Septal Perforation: Simultaneous Rhinoplasty and Septal Perforation Repair - October 1, 2014

It was reported that actor Zac Efron fractured his jaw in a fall, requiring surgical repair. In order to help the fracture heal, surgeons deemed it necessary to wire his jaw shut. This extreme step is traditionally required to improve wound healing. However, given how painful and disabling jaw wiring is, any alternative effective options should be sought.
Currently, there are a few surgeons who are able to repair jaw fractures without wiring. Experts in facial trauma surgery can repair jaw fractures and avoid prolonged jaw immobilization, resulting in an easier recovery with less pain and fewer complications.
Why is the jaw wired closed when it is fractured?
When a bone is broken anywhere in the body, immobilization is an important part of treatment. When broken bones are allowed to move, they do not set correctly, resulting in dysfunction of the bone and chronic pain at the fracture site. Just like a broken arm is placed in a cast to prevent movement, the fractured jaw also must be immobilized. However, rather than using a cast, in the fractured jaw, wires are used to stabilize the broken jaw against the healthy upper jaw. This process is called mandibular-maxillary fixation (MMF) and it prevents the fractured jaw segments from moving with swallowing and chewing. After an extended period of immobilization (usually 6-8 weeks), the jaw is considered healed and the wires are removed.
What are the risks of jaw immobilization with wiring?
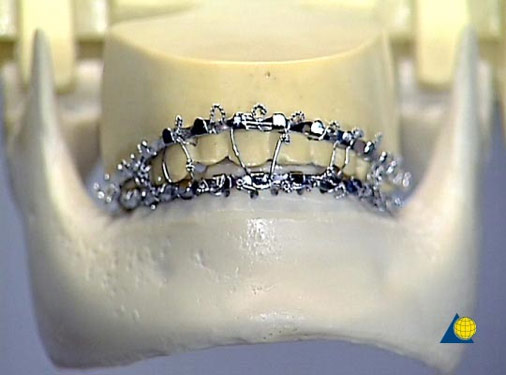
Wiring of the jaw, called mandibular-maxillary fixation (MMF), is used to prevent the fractured jaw segments from pulling apart during normal oral tasks (i.e.,. chewing). This is done for a period of 6-8 weeks, during healing. Unfortunately, jaw wiring does carry several potential complications. When the jaw is wired shut, it is a risk to the airway, presenting a choking hazard. If a wired patient were to vomit or was choking, the mouth would be incapable of opening, resulting in a life-threatening situation. In addition, immobilization of the jaw commonly results in temporomandibular joint (TMJ) issues, leading to lifelong jaw popping, pain, or dislocation.

Equally relevant is the fact that during this period of immobilization, the patient is limited in their ability to communicate, work, eat, and drink. The teeth are constantly clenched against each other, making normal oral functions impossible.
The short-term disabilities and long term complications of MMF are severe.
For these reasons, it is critical to seek an alternative to MMF if one is available.
What is the best treatment of a jaw fracture?
Jaw fractures must be repaired surgically. Stabilization of the jaw is accomplished by attaching thin undetectable plates to the bone fragments. A surgeon strategically places these plates through small incisions made along the gum line, avoiding any facial scars. The upper and lower jaws are wired to each other, to prevent the jaw segments from moving.
Ideally, to avoid complications of prolonged jaw immobilization, wiring should not be performed. However, there are few surgeons who are able to successfully treat jaw fractures without wiring. When performed by an expert in facial trauma surgery, wiring can be successfully avoided, allowing the patient to return to normal function significantly earlier. Also, the health risks of jaw joint disorders are thereby avoided.
The physicians of the Osborne Head and Neck Institute (OHNI) are facial trauma experts, possessing dual board certifications in otolaryngology and plastic/reconstructive surgery. This unique combination of training allows them to address both the functional and cosmetic concerns of facial trauma. In addition, the doctors of OHNI are known internationally for their high success rate in treating jaw fractures without traditional jaw wiring techniques. These cutting edge techniques have allowed patients to retain a high quality of life during healing while avoiding the extended discomfort and permanent disability of traditional techniques.
For more information on jaw fracture evaluation please contact the Osborne Head and Neck Institute.