- Scar Revision for Surgical, Traumatic, and Keloids Scars - January 6, 2020
- Hereditary Hemorrhagic Telangiectasia - May 25, 2016
- Hereditary Hemorrhagic Telangiectasia: Septal Perforation and Nose Bleeds - May 23, 2016
- Hereditary Hemorrhagic Telangiectasia: Epistaxis and Septal Perforation - May 18, 2016
- Wegener’s Granulomatosis: Autoimmune Disease and Multi-Focal Septal Perforation - May 9, 2016
- Kyle Korver: Facial Injury and Nasal Fracture - March 24, 2015
- Russell Westbrook: Facial Injury and Surgery - March 5, 2015
- Mega-perforation: Pushing the Limits of Septal Perforation Repair - November 26, 2014
- Septoplasty Complication and Septal Perforation - November 24, 2014
- Nose Picking (Rhinotillexis) and Septal Perforations: Why I should stop picking my nose…? - November 24, 2014
- Nasal Fractures, Septal Hematoma, and Septal Perforation: Simultaneous Rhinoplasty and Septal Perforation Repair - October 1, 2014
What is Scar Revision?
Scar Revision refers to a procedure that reduces the appearance of scars by matching them to the texture and color of the surrounding skin. It also helps improve function by releasing scar tissue, thereby returning movement to an area of the body (fingers, nose, mouth, eyelids) that may have been tethered by scar tissue.
Why Do People Get Scar Revision?
There are many reasons to consider scar revision. These include:
- Irritation: scars can be itchy, tender, and painful
- Function: scar tissue is less flexible and can inhibit function or movement
- Appearance: scars can make people feel self-conscious, anxious or depressed
Surgical Scars:
Surgical scars can be planned to minimize their appearance, size, and risk of resultant tissue dysfunction. However, some patients heal poorly from even a planned surgical incision and desire scar revision. Post-surgical treatments can be used first to reduce scar size and avoid the need for another surgery. Avoiding the sun or using strong sunblock for a year after surgery will limit hyperpigmentation of the scar. Compression over the scar can reduce hypertrophic scarring, which is when excess collagen accumulates and produces a raised scar. This can be done through taping, gently massaging, or using silicone gel and sheets. However wide, thick, or hyperpigmented scars can still form even if proper post-surgical treatments are implemented. In these cases, scar revision can be considered.
Burn Scars:
Burns may be initially treated with skin grafts, which is the use of healthy donor skin from elsewhere on the body to cover the burn site.
Donor Sight of the Skin Graft The FDA approved clinical trials for “spray-on skin” in September of 2018. Named ReCell (Avita Medical, Valencia, California), this new technology is an example of an early skin cell regenerator. It enables doctors to produce a suspension of cells by culturing a sample of the patient’s own skin. This suspension contains the cells necessary to regenerate the outer layer of natural, healthy skin and is prepared and applied at the point-of-care in as little as 30 minutes. This could prove an exciting new option in the treatment of burns that will spare the patient the pain of healing a donor site wound.
Keloids:
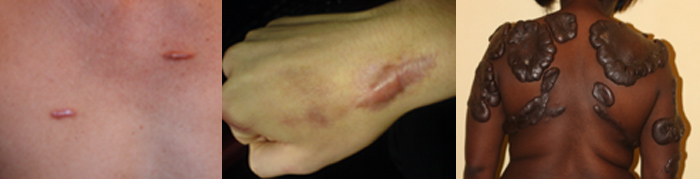
What Are Keloids?
Keloids are raised bumpy scars that form from excess collagen production at the site of tissue trauma. This can happen due to surgery, an accident, or something as simple as ear-piercing in the susceptible individual.
Keloids can be itchy and tender for some people when they are forming, but the itch stops once the Keloid stabilizes. If a keloid does form on a joint it can restrict movement.
People of color are more prone to develop keloids. People under 30 are also at a higher risk. They can appear anywhere on the body; however, keloids are more common on the face, neck, ears, chest or shoulders where there is little underlying fatty tissue.
Keloids can be painful, itchy, uncomfortable, unsightly and bothersome. People can undergo scar revision to help make these less visible or irritating.
Scar Revision for Keloids:
Removal of the keloid is not advised because the trauma from the incision will simply result in another keloid, and often one that is larger. Alternatives include:
- Cryotherapy: freezing the keloid using liquid nitrogen
- Steroid injections: might decrease itchiness, burning, and redness. It might also help to flatten the keloid and, in some cases, make them smaller.
- Laser surgery done in conjunction with other treatments can smooth the keloid, reduce discoloration, or flatten the keloid.
- Topical silicone treatment
- External beam radiotherapy: typically performed in conjunction with a surgical excision for refractory keloids