- Hereditary Hemorrhagic Telangiectasia - May 25, 2016
- Hereditary Hemorrhagic Telangiectasia: Septal Perforation and Nose Bleeds - May 23, 2016
- Hereditary Hemorrhagic Telangiectasia: Epistaxis and Septal Perforation - May 18, 2016
- Wegener’s Granulomatosis: Autoimmune Disease and Multi-Focal Septal Perforation - May 9, 2016
- Kyle Korver: Facial Injury and Nasal Fracture - March 24, 2015
- Russell Westbrook: Facial Injury and Surgery - March 5, 2015
- Mega-perforation: Pushing the Limits of Septal Perforation Repair - November 26, 2014
- Septoplasty Complication and Septal Perforation - November 24, 2014
- Nose Picking (Rhinotillexis) and Septal Perforations: Why I should stop picking my nose…? - November 24, 2014
- Nasal Fractures, Septal Hematoma, and Septal Perforation: Simultaneous Rhinoplasty and Septal Perforation Repair - October 1, 2014
Body piercing has become more popular and less taboo in recent years. With an increase in piercing there has been a concomitant increase in complications .One area particularly at risk is the human ear. Anatomic and physiologic features of the ear make it especially prone to injury and infection.
The human ear is composed mainly of a cartilaginous framework. Cartilage is a very strong and flexible material that can provide structural support as well as flexibility. In order to achieve these characteristics, blood vessels and nerves are not found within cartilage tissue. Due to the lack of dedicated blood supply, cartilage is one of the body’s only tissues that must derive nutrients from its overlying tissue. Perichondrium tightly surrounds cartilage and is responsible for providing metabolic support and nutrients across its cells to neighboring cartilage tissue.
When injuries occur that damage the perichondrium, underlying cartilage is susceptible to permanent tissue damage and possible disfigurement.
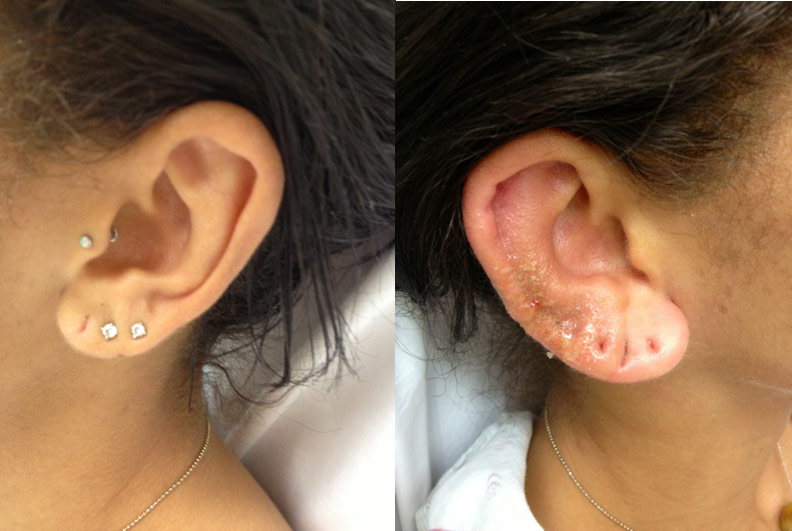
What is perichondritis?
Perichondritis is simply, inflammation of the perichondrium, the thin tissue that provides oxygen and nutrient exchange to the underlying cartilage. When perichondritis occurs in the ear it is commonly referred to as auricular perichondritis.
How does someone get perichondritis of the ear?
Perichondritis can occur due to a variety of different causes that injure the delicate perichondrium including:
- Cartilage piercings
- Surgical trauma
- Physical trauma from contact sports or physical altercations
- Animal or insect bites
Currently, the most common cause of auricular perichondritis is infection due to piercing of the ear’s cartilage. Unsterile piercing technique can easily introduce bacteria into the perichondrial tissues leading to inflammation, tissue damage, gangrene, and subsequent complications.
What are the symptoms of perichondritis?
Perichondritis can initially look like a simple skin infection or irritation characterized by a red and inflamed area around a piercing or point of trauma. As time passes infection can pass from the overlying perichondrium to the deeper layers of cartilage, causing the affected area to become firm and very tender. In advanced cases, the skin can begin to darken, produce discharge, and breakdown.
Why is it important to seek prompt evaluation of suspected perichondritis?
Perichondritis can appear benign and inconsequential in its initial stages. What is not readily evident is that as inflammation sets in, the perichondrium is being separated from the underlying cartilage. This results in a barrier to nutrient exchange between the two structures and eventual cartilage tissue damage (chondritis). If bacteria have also gained access to the underlying cartilage, it too will cause tissue death through separate mechanisms, leading to severe deformities.
The goal of prompt treatment is to prevent prolonged perichondrial inflammation as well as infection and death of the underlying cartilage. If evaluation and treatment are delayed in these cases, perichondritis can progress to chondritis and subsequent tissue death. Portions of the ear that have been irreversibly damaged require surgical removal. In some cases this procedure can result in distortion of the ears natural shape resulting in disfigurement or unwanted cosmetic changes and necessitating reconstructive surgery.
Who should evaluate and treat all cases of suspected perichondritis?
All cases of suspected perichondritis should be promptly evaluated and treated by a qualified facial trauma specialist. These specially trained physicians are experts in recognizing and treating injuries and complications related to the face and ears. In addition, facial trauma specialists can recognize and address the functional concerns of the ear while preserving the aesthetic appearance of the ear and face.
To learn more about Dr. Jason Hamilton or perichondritis, please visit www.facialtraumamd.com.