- New Sublingual Allergy Tablets - October 31, 2014
- Ground-breaking New Treatment Option for Sleep Apnea - September 27, 2014
- Allergies versus Viruses in Children - September 27, 2014
- “Dog Dust” Protects Children from Allergies - September 27, 2014
- Nasal Saline Irrigation - August 8, 2014
- Doctor, I am Allergic to Dust. What Can I do? - July 31, 2014
- Infants Exposed to Dust Mites Less Likely to Develop Allergies - June 23, 2014
- How to Treat a Young Child’s Cough - December 17, 2013
- Many Parents are Unaware That Their Children Are at Risk for Noise Induced Hearing Loss - December 9, 2013
- Is it a Cold or an Ear Infection? - December 9, 2013
Question: My child always has a runny nose. Can my child be tested for allergies?
I recently brought my 3 year old daughter to the pediatrician because she has had a runny nose for months. She is not sick, but almost always has mucous coming out of her nose. She sometimes develops a cough as well. She does not act sick and doesn’t develop a fever. The pediatrician think it may be allergies. Is there a way to find out if my child has allergies?

Discussion:
The child with the runny nose is a common sight to parents. When the nose starts running, we know that a cold is right around the corner. But what may be just as bothersome is the child whose nose is always running, even when they are not sick. They may even mouth breathe because of nasal congestion.
Runny noses are most commonly due to a cold (viral infection), sinusitis (bacterial infection) or allergies.
It is sometimes hard to distinguish between these, especially if a child always has a runny nose. A constantly runny nose is most often due to allergies but may also be due to anatomic problems, like enlarged adenoids. A pediatric otolaryngologist is best able to help you determine the cause of your child’s runny nose.
If allergies are suspected, allergy testing can be performed to determine what a child is allergic to. Allergy testing can be done by skin testing or blood testing. Blood testing involves a needle stick, which is very difficult to perform in children. The advantages of skin testing are that:
- It can be done in the office
- Results are available the same day
- It does not require needles or shots
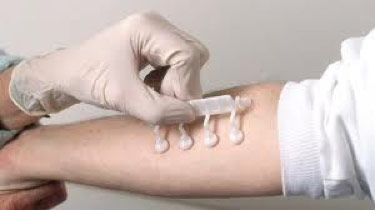
Skin testing involves placing the allergens (possible causes of allergies, such as dogs, cats, trees, etc) on the skin with a plastic device. The allergens are placed on either the forearms or the back and are left in place for 20 minutes. It is very routine and easily tolerated. Indeed, the hardest part of skin allergy testing is trying to help your child not touch the test sites! After 20 minutes, the skin is inspected for a reaction.
Allergy testing checks for responses to the most common allergens in your area, including weeds, grasses, trees, animals, dust, and molds. If you child is allergic to something that is present all year round, such as dust (or your pet), this may explain a constantly runny nose.
 If allergy testing is positive, you may consider treatment options including:
If allergy testing is positive, you may consider treatment options including:
- Environmental (controlling your child’s exposure to their allergen)
- Nasal sprays (saline, antihistamines and steroid)
- Antihistamine pills/syrups (i.e., Claritin, Allegra, etc)
- Immune therapy (shots or sublingual therapy)
Many parents are concerned about their children being on medications. However it is important to start treatment of allergies and get your child breathing through their nose. The risks of untreated allergies include:
- Constant runny nose
- Nasal obstruction
- Mouth breathing with changes to the shape of the face due to the mouth being open (called “adenoid facies”)
- Frequent colds
- Frequent coughs
- Ear infections
- Asthma/reactive airway disease
In some cases it is possible to limit how long your child is on medication based on the allergy test results. It is also important to know that a child’s allergic profile can change over time so as a child ages or symptoms change repeat allergy testing may be recommended. Your pediatric otolaryngologist can discuss testing and treatment options with you.