- Graves’ Disease: General Overview - September 25, 2017
- The Effect of Bulimia on the Parotid Gland - September 25, 2017
- Graves’ Disease: Treatment Overview - September 25, 2017
- Question: How do the ingredients in e-cigarettes and vaporizers affect respiratory health? - August 16, 2019
- Bad Technique and Vocal Injury - January 9, 2019
- Is Edible Marijuana Dangerous for the Voice? Myths Dispelled - December 18, 2018
- Surprise! You have a hemorrhage - January 31, 2018
- Graves’ Disease: Treatment Overview - September 25, 2017
- Adele and the Stigma of Vocal Injury - July 11, 2017
- Vocal Curbside Consult: How does the thyroid affect the voice? - May 16, 2017
- Vocal Curbside Consult: How do hormones affect the voice? - May 3, 2017
- Vocal Curbside Consult: How do emotion and stress affect the voice? - April 17, 2017
- Vocal Curbside Consult: Vocal Recovery After Illness - April 7, 2017
Graves’ Disease is an autoimmune disease that results in the overproduction of thyroid hormones, or hyperthyroidism. Graves’ Disease patients produce an antibody that interferes with the normal operation of their thyroid gland. These antibodies, called Thyroid Stimulating Immunoglobulins (TSI) bind to receptor cells in the thyroid gland, resulting in hyperthyroidism, or elevated thyroid hormone levels. Left untreated, Graves’ Disease can be fatal due to severe metabolic dysregulation.
There are three methods used to treat Graves’ Disease: Anti-Thyroid Drugs (ATD), Radioactive Iodine Ablation (RAI), and surgery to remove a portion or all of the thyroid gland. Each method has advantages as well as limitations therefore treatment plans are personalized.
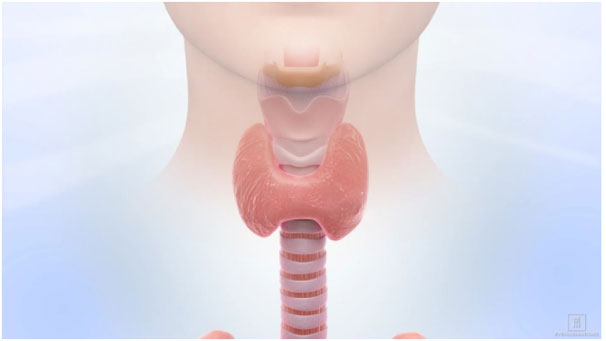
It is common for patients to seek initial treatment with Anti-Thyroid Medications because they are not invasive like surgery and do not harbor any of the concerns surrounding radioactivity. The two medications used are Methimazole and Propylthiouracil. Neither drug cures Graves’ Disease; however, both function to combat the symptoms of hyperthyroidism by interfering with the thyroid’s ability to use iodine to produce hormones. The medications are not typically recommended past 2 years and are generally taken until Graves’ goes into spontaneous remission or a more definitive treatment plan is determined. Otherwise, the medications can serve as a supplement to Radioactive Iodine Ablation.
Complications with the medication often indicate the need for further treatment. The most common complication is failure of the medication to effectively treat a patient’s symptoms. Other indications may include allergies to the medication or an aversion to the side effects such as rashes, joint pain, liver failure, and increased susceptibility to infection. Propylthiouracil has been known to cause liver failure in pediatric cases and Methimazole poses the risk of birth defects in pregnant women.
Radioactive Iodine Ablation (RAI) is the most commonly used treatment method for adults in the United States because it is conveniently taken orally in capsules. The iodine enters the thyroid gland and the radioactivity destroys the overactive thyroid cells over time which causes symptoms to gradually lessen. The treatment typically requires several weeks or months and may involve a temporary period of heightened symptoms, particularly the exophthalmos (bulging eyes). For this reason, RAI is not typically recommended for patients with severe cases of the exophthalmos. RAI is also rarely recommended for pediatric patients because of concern surrounding prolonged exposure to radioactivity; however, the most extensive research to date shows no increase in the likelihood of cancer or genetic defects. Women who are pregnant and/or nursing are often recommended to avoid RAI in an effort to decrease their exposure to radioactivity. In all patients RAI eventually destroys the entire thyroid gland. This means lifetime hormone supplementation is necessary to replace the hormones typically produced by the thyroid. These supplements are taken daily in the form of oral capsules.
Surgery is the fastest, most efficient, and most permanent method of treating Graves’ Disease. It does, however, involve risks. With the partial removal of the thyroid gland in a subtotal thyroidectomy, the remaining thyroid can resume the function of hormone production; therefore no supplements will be needed. It may, however, not entirely eliminate symptoms and will increase the likelihood of recurrence. A total thyroidectomy will require a lifetime of thyroid hormone replacement; however, it eradicates the symptoms and possibility of recurrence. The amount resected is primarily dependent on the severity of the Graves’ Disease.
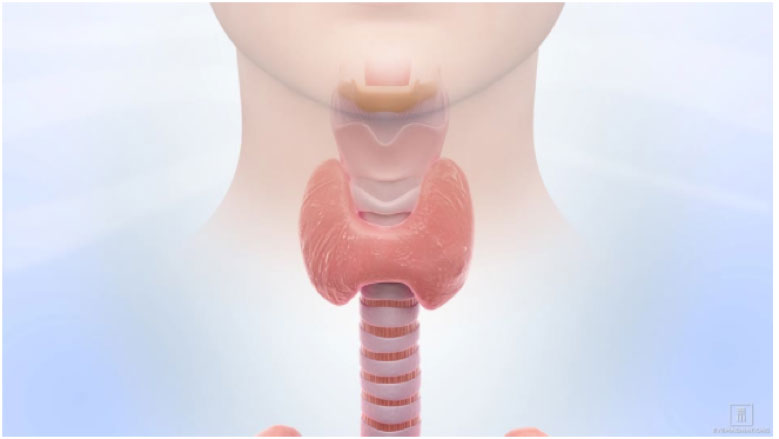
The complications of surgery include potential damage of the parathyroid glands, which are adjacent to the thyroid gland and serve to regulate calcium levels in the blood. An injury to the parathyroid glands may result in hypocalcemia, or calcium deficiency, that must be treated with calcium, temporarily or permanently. Other risks include possible damage of the recurrent laryngeal nerve which can result in vocal cord paralysis causing symptoms such as hoarseness, noisy breathing, loss of vocal pitch, inability to speak loudly, loss of gag reflex, and coughing or choking while swallowing.
Treatment of Graves’ Disease should only be managed by specialized and experienced physicians that can manage the aforementioned concerns and safeguard the patient’s quality of life.
To learn more about Graves’ Disease of thyroid surgery, please visit: www.ohni.org.