- Question: How do the ingredients in e-cigarettes and vaporizers affect respiratory health? - August 16, 2019
- Bad Technique and Vocal Injury - January 9, 2019
- Is Edible Marijuana Dangerous for the Voice? Myths Dispelled - December 18, 2018
- Surprise! You have a hemorrhage - January 31, 2018
- Graves’ Disease: Treatment Overview - September 25, 2017
- Adele and the Stigma of Vocal Injury - July 11, 2017
- Vocal Curbside Consult: How does the thyroid affect the voice? - May 16, 2017
- Vocal Curbside Consult: How do hormones affect the voice? - May 3, 2017
- Vocal Curbside Consult: How do emotion and stress affect the voice? - April 17, 2017
- Vocal Curbside Consult: Vocal Recovery After Illness - April 7, 2017
 When a professional voice user complains of vocal symptoms, they may be suffering from “strain” or “muscle tension dysphonia.” This is not a specific diagnosis; rather, it refers to how the voice is being used. Muscle tension dysphonia (MTD) is the technical term for stressful or strenuous overuse of the voice, resulting in vocal dysfunction. Over time, untreated MTD results in worsening of symptoms, including loss of vocal range and pain when singing/performing.
When a professional voice user complains of vocal symptoms, they may be suffering from “strain” or “muscle tension dysphonia.” This is not a specific diagnosis; rather, it refers to how the voice is being used. Muscle tension dysphonia (MTD) is the technical term for stressful or strenuous overuse of the voice, resulting in vocal dysfunction. Over time, untreated MTD results in worsening of symptoms, including loss of vocal range and pain when singing/performing.
What are the symptoms of MTD?
Symptoms can vary but generally the following changes may be observed:
- Rough or hoarse voice
- Deepening of the voice
- Difficulty projecting
- Throat pain with use, especially while performing
- Vocal fatigue
- Sudden changes in pitch
- Sense of strained or effortful voice
- Voice quality that worsens with use but recovers with rest
What is MTD?
Muscle tension dysphonia means that there are muscles being used for sound production (phonation) that should not be used. During normal, healthy vocalization, only the vocal cords should move. However, in MTD, other muscles including the false vocal folds, the laryngeal strap muscles (in the neck), and the sternocleidomastoid muscles are used to produce or support sound.
These patterns of muscle misuse may develop for many reasons. Some untrained voices naturally rely on accessory muscle use because that is the only way they can produce the desired sound or power. Some people with excellent training develop MTD as a result of a temporary injury (i.e., laryngitis, a cold, etc). The injury forces the singer to use their voice differently to compensate, but after recovery the pattern of muscle misuse persists.
Who is at risk for MTD?
MTD can occur for medical or non-medical reasons. An example of a non-medical source of MTD is improper vocal training. The untrained voice will use the wrong support methods to vocalize, resulting in strain, or MTD. Medical issues that can potentially contribute to developing MTD include:
- Weakness (paresis) of the vocal folds
- Paralysis of the vocal folds
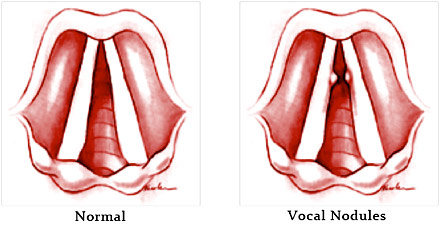
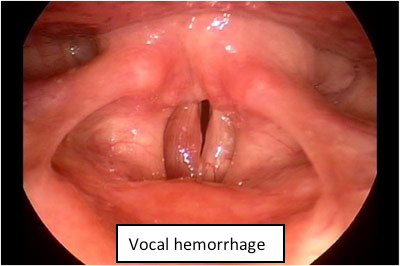
- Vocal hemorrhage, polyps, cysts, nodules
- Irritation from smoking, infection, or reflux
- Mood issues such as anxiety and depression
- Stress
How is MTD evaluated?
To determine if you suffer from MTD, evaluation by an experienced laryngologist is recommended. Laryngology is a medical subspecialty that is obtained after otolaryngology (ENT) training has been completed. Only a laryngologist possesses the specialized and focused training that is critical for the comprehensive evaluation of vocal pathology.
During your evaluation a laryngologist will use cutting edge technology including stroboscopy and flexible laryngoscopy to visualize the function of your laryngeal muscles and vocal folds. These skilled diagnostics allow a specialist to effectively observe any dysfunction or abnormality that may be present in generating voice.
What does MTD Look Like?
MTD can sometimes be seen externally as visibly tight or straining muscles of the neck during singing or speaking. It is also common for there to be no external signs of MTD. For these reasons, a laryngologist will use an endoscope to directly visualize the function of your laryngeal muscles and vocal folds during speech. In MTD, the laryngologist will note that muscles normally tasked with phonation are not being used effectively. Instead, compensatory muscles are abnormally active and tense.
What is the risk of untreated MTD?
Untreated MTD carries several potential risks. Continued straining of the vocal folds can lead to injury, such as hemorrhage or nodule formation. In severe cases of chronic straining, permanent damage to the vocal folds may occur. Early diagnosis and treatment by a vocal specialist (laryngologist) can prevent the complications seen in untreated MTD.
What are the treatment options for MTD?
The gold standard therapy for MTD is voice therapy from a qualified voice therapist. Voice therapy is a specialty within the field of speech and language pathology focusing on the treatment of vocal disorders. A voice therapist works with patients to modify the method of voice production, promote vocal fold healing, and remove harmful vocal habits. In addition, a vocal therapist will customize a treatment plan around a patient’s unique issues and capabilities.
Dr. Reena Gupta, director of the Division of Voice and Laryngology at the Osborne Head and Neck Institute is a board certified otolaryngologist and has completed subspecialty training in the field of laryngology. Dr. Gupta’s advanced specialty training and extensive clinical experience have placed her in a unique position to comprehensively evaluate and treat the voice and voice disorders.
For more information on muscle tension dysphonia please contact the Osborne Head and Neck Institute.



